Continued Enrollment Growth in Employer-Group Medicare Advantage
October 31, 2018
As of October 1, 2018, total Medicare Advantage (MA) membership stood at over 21 million, representing approximately 34% of the 63.3 million Americans eligible for Medicare. Medicare Advantage plans can either be acquired individually through direct purchase policies or through employer/group retiree programs, commonly known as Medicare Advantage Employer Group Waiver Plans (MA-EGWPs). Since the inception of Medicare Advantage in 2003, Individual MA policies have historically dominated the market as 17.1 million beneficiaries purchased MA plans as of October 1, 2018. However, despite a decrease over the years in the number of private sector employers offering retiree health benefits, membership trends in MA-EGWPs have demonstrated notable enrollment growth, especially within the past two years.
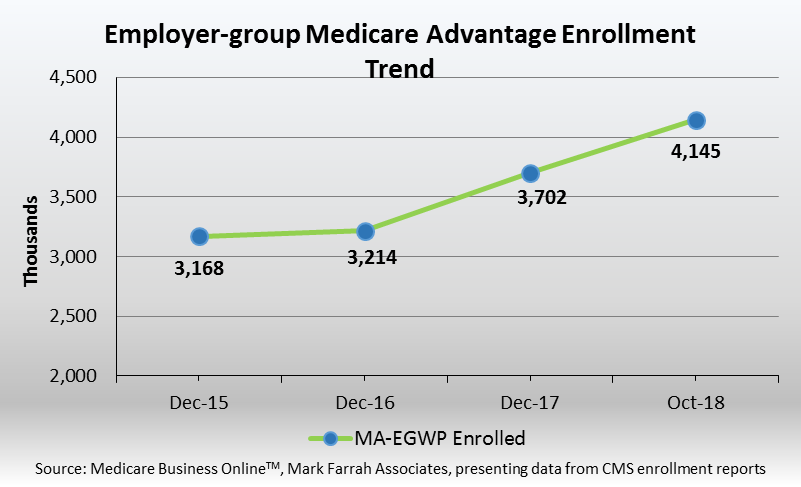
Since December 2017, employer-group Medicare Advantage enrollment has increased by over 443,000. In fact, over the past four years, group market enrollment has increased by approximately 1 million members, nearly a 125% increase in membership since December 2015. This brief provides insights about the current employer-group Medicare Advantage market and assesses membership trends over the past four years by carrier and state.
Enrollment Trends by Carrier and State
According to the Centers for Medicare and Medicaid Services (CMS) Medicare Advantage enrollment reports aggregated by Mark Farrah Associates in Medicare Business Online™, approximately 4.1 million, or 19%, of total Medicare Advantage members originated through an employer-group health plan as of October 2018. Group membership continues to grow, as roughly 443,000 more beneficiaries were enrolled in employer-group MA plans than in December of 2017, a 12% increase.
The top five carriers covered nearly 82% of all group Medicare Advantage enrollees as of October 1, 2018. Growth in UnitedHealth plans was the primary driver of overall enrollment gains with approximately 1.3 million group plan members to date. Aetna added 148,000 group members so far in 2018, coming close to matching UnitedHealth’s gains, bringing their total group enrollment to just shy of 700,000. Kaiser Foundation Group trailed UnitedHealth and Aetna’s employer-group MA membership with 536,000. Humana and Blue Cross Blue Shield of Michigan also command a sizeable share in the Group Medicare market with both carriers experiencing notable growth thus far in 2018.
| Top 5 Medicare Advantage Payers - Group Segment Membership Trend |
||||
|---|---|---|---|---|
| Company | Dec-15 | Dec-16 | Dec-17 | Oct-18 |
| UnitedHealth | 670,833 | 789,377 | 1,148,615 | 1,297,212 |
| Aetna | 538,562 | 563,938 | 547,618 | 696,088 |
| Kaiser | 472,433 | 486,115 | 525,711 | 536,272 |
| Humana | 469,019 | 341,926 | 428,240 | 484,260 |
| BCBS of Michigan | 282,661 | 302,207 | 318,675 | 371,571 |
| Total | 2,443,508 | 2,483,563 | 2,968,859 | 3,385,403 |
Source: Medicare Business OnlineTM, Mark Farrah Associates, presenting data from CMS enrollment reports
As shown in the table above, all leading health plans with group Medicare Advantage realized overall increases in membership since December 2015. UnitedHealth experienced the largest increase, adding over 626,000 members for a net gain of 93%. Aetna experienced the second largest growth with approximately 158,000 new enrollees for a net gain of 29%. The overall net gain between 2015 and 2018 for the top five companies was 952,000 members, or 39%.
Total net membership increased 31% nationally between December 2015 and October 2018 as illustrated in the chart below. Employer-group Medicare Advantage market penetration varies across states, but enrollment trends indicate growth in most states since 2015 within the U.S. and its surrounding territories. The ten states with the highest Group Medicare enrollment experienced membership increases except for Ohio. Having the highest percentage of enrollees with over 586,000 members, California saw a 21% enrollment increase since December 2015. Of the leading states, Texas and Florida saw the most membership gains with increases of 60% and 53% respectively.
| Top 10 States Medicare Advantage - Group Segment Membership Trend |
||||
|---|---|---|---|---|
| State | Dec-15 | Dec-16 | Dec-17 | Oct-18 |
| CA | 485,136 | 522,411 | 552,221 | 586,815 |
| MI | 300,280 | 315,917 | 333,653 | 392,375 |
| TX | 196,871 | 211,098 | 244,097 | 315,504 |
| NY | 216,737 | 221,630 | 250,598 | 263,331 |
| OH | 315,820 | 191,397 | 204,936 | 236,634 |
| PA | 203,375 | 201,425 | 216,773 | 218,825 |
| IL | 150,448 | 162,023 | 189,044 | 200,304 |
| NC | 129,959 | 139,685 | 154,050 | 177,884 |
| FL | 106,356 | 110,619 | 139,670 | 162,334 |
| GA | 131,398 | 137,122 | 150,051 | 160,804 |
| Subtotal | 2,236,380 | 2,213,327 | 2,435,093 | 2,714,810 |
| All Other States | 931,945 | 1,000,234 | 1,266,598 | 1,430,199 |
| Total | 3,168,325 | 3,213,561 | 3,701,691 | 4,145,009 |
Source: Medicare Business OnlineTM, Mark Farrah Associates, presenting data from CMS enrollment reports
A Look Ahead
Medicare Advantage plans continue to be an attractive option for the growing senior population. Consequently, this presents increasing opportunities for state governments and employers as MA employer-group plans help maintain consistent, high-quality health coverage at lower costs for their Medicare-eligible retirees. Further, this market continues to afford growth opportunities for health companies with business in this competitive segment.
However, regulatory changes could threaten the financial stability of MA employer-group health plans. As noted in the 2019 Call Letter, the Centers for Medicare and Medicaid Services (CMS) is proposing to fully transition to a new payment system that replaces the MA-EGWP bidding system with a fixed payment system based on a county benchmark of average individual MA plan bids. There are concerns regarding this methodology and CMS continues to solicit comments as it seeks to refine and finalize this policy.
About Mark Farrah Associates (MFA)
Mark Farrah Associates (MFA) is a leading data aggregator and publisher providing health plan market data and analysis tools for the healthcare industry. Our product portfolio includes Health Coverage Portal™, County Health Coverage™, Medicare Business Online™, Medicare Benefits Analyzer™, and Health Plans USA™. For more information about these products, refer to the informational videos and brochures available under the Our Products section of the website or call 724-338-4100.
Healthcare Business Strategy is a free monthly brief that presents analysis of important issues and developments affecting healthcare business today. If you would like to be added to our email distribution list, please submit your email to the "Subscribe to MFA Briefs" section in the grey area at the bottom of the page.