Mid-Year Trends in Health Insurance Enrollment and Segment Performance
September 30, 2020
While the health insurance industry is accustomed to volatility due to policy issues and an ever-changing competitive landscape, the spread of COVID-19 has undoubtedly impacted many additional aspects of the health care ecosystem. It is no surprise that insurers are seemingly poised to weather this disruption and appear committed to adapting to these new challenges. However, despite the calamity caused by the pandemic, enrollment for the second quarter of 2020 increased in most health insurance segments.
Based on data filed in statutory financial reports from the NAIC (National Association of Insurance Commissioners) and the CA DMHC (California Department of Managed Health Care), 274 million people received medical coverage from U.S. health insurers, as of June 30, 2020. This number is up from 268.2 million, or approximately 5.8 million members, from a year ago. Mid-year enrollment trends indicated membership gains for Individual, Medicare Advantage (MA), Managed Medicaid, and Employer-Group ASO (administrative services only for self-funded plans) business, while the Employer-Group risk segment experienced a year-over-year decline. In this brief, Mark Farrah Associates (MFA) assessed the latest year-over-year enrollment trends, comparing second quarter 2019 with second quarter 2020 segment membership.
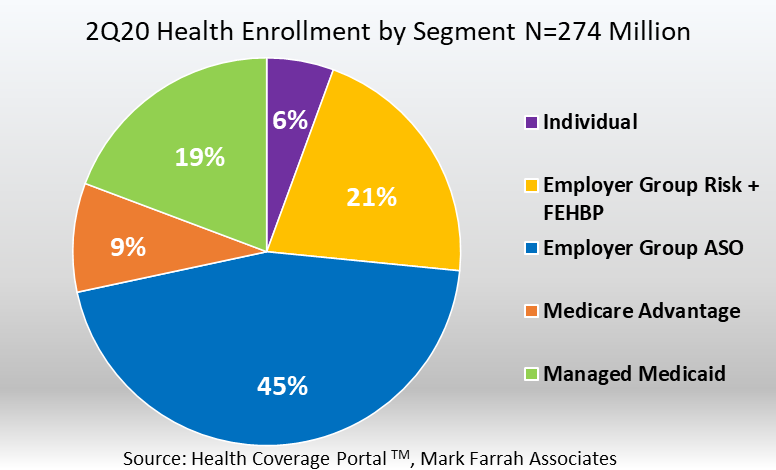
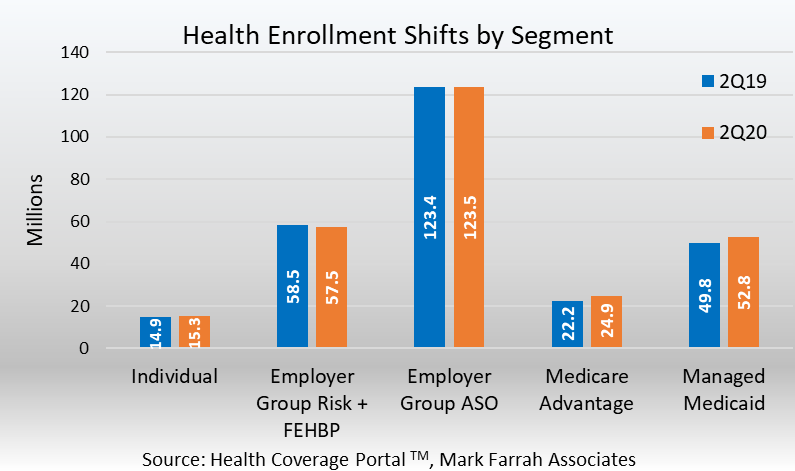
- The individual market has seemingly weathered the storm during the early years of ACA and has stabilized into a health segment for insurers. COVID-19 has not presented major challenges for the segment so far for 2020. With this stability, some insurers are increasing their geographic footprint for ACA-compliant plans for 2021. In June 2020, health insurers reported total individual, non-group coverage for over 15.3 million people, this represents a 2.8% increase, or 420,000 members, from 14.9 million in June 2019. The first year over year increase since 2015 for the segment. Open enrollment for 2021 coverage starts on Nov. 1st and runs through Dec. 15th, although some states, including New York, California and Massachusetts have permanently extended their open enrollment periods.
- According to figures from Centers for Medicare & Medicaid Services (CMS), nearly 73.5 million individuals were enrolled in Medicaid and the Children’s Health Insurance Program (CHIP), as of May 2020. For Managed Medicaid, based on data filed in statutory financial reports, approximately 52.8 million beneficiaries received healthcare through Managed Care Organizations (MCOs) in second quarter 2020. This is an increase of 5.9%, or 2.9 million enrollees from 2Q19 to 2Q20.
- Medicare Advantage (MA) continues to experience enrollment gains as MA plans, with extra benefits and services at lower costs over original Medicare, remain appealing to seniors. Although MA market penetration is strong, there is still ample opportunity for growth with only 36% of the nearly 70 million people eligible for Medicare enrolled in MA plans. As of June 30, 2020, Medicare Advantage experienced membership increases as over 2.6 million more seniors chose an MA plan from the same period a year ago. According to plan-reported statutory reports, enrollment in MA plans grew from 22.2 million in June of 2019 to over 24.8 million in June 2020. This is a sizable increase of 11.9% growth, due to the significant number of seniors entering retirement each day.
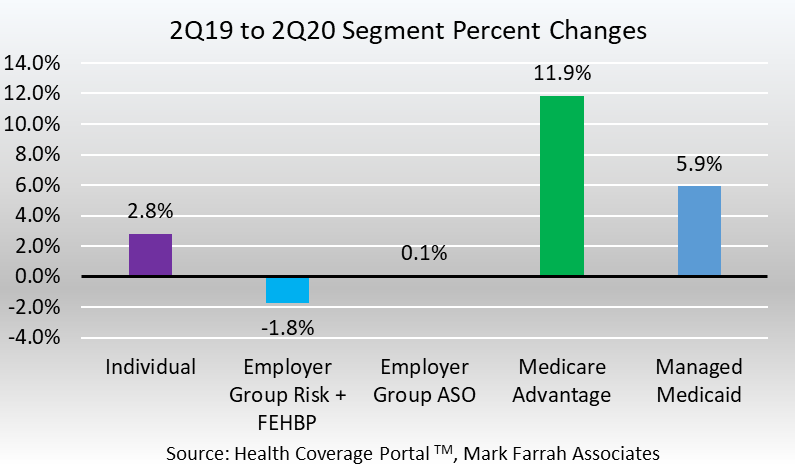
- Employer-Groups continue to be the leading source of health coverage in the U.S. The latest figures show Employer-Group risk membership, including Federal Employees Health Benefit Plans (FEHBP) enrollment, experienced a decrease of 1.8% between 2Q19 and 2Q20. This is a year-over-year decrease of over 1 million lives. Mid-year Group-risk enrollment stood at 57.5 million as compared to 58.5 million in June of 2019. While, many companies have shifted towards self-funded (ASO) insurance, in the years since the implementation of the ACA, to help control costs and improve the health and well-being of its employees, employee layoffs due to the COVID-19 economic downturn are also a cause of this decrease.
- According to MFA’s recent estimates, Employer-Group ASO (administrative services only for self-funded business) membership grew by 68,000 members from June 2019 to June 2020. MFA identified 123.5 million ASO covered lives, which encompassed 45% of total health enrollment for 2Q20.
About the Data
The data used in this analysis brief was obtained from Mark Farrah Associates' Health Coverage Portal™ database. Employer group ASO figures may be estimated by Mark Farrah Associates using credible company and industry resources. Individual, Non-Group membership reported by some carriers may include CHIP (Children’s Health Insurance Program). These adjustments may have resulted in moderate understatement or overstatement of enrollment changes by segment. Findings reflect enrollment reported by carriers with business in the U.S. and U.S. territories. Data sources include NAIC (National Association of Insurance Commissioners) and the CA DMHC (California Department of Managed Health Care). As always, MFA will continue to report on important plan performance and competitive shifts across all segments.
About Mark Farrah Associates (MFA)
Mark Farrah Associates (MFA) is a leading data aggregator and publisher providing health plan market data and analysis tools for the healthcare industry. Our product portfolio includes Health Coverage Portal™, County Health Coverage™, Medicare Business Online™, Medicare Benefits Analyzer™, 5500 Employer Health Plus™, and Health Plans USA™. For more information about these products, refer to the informational videos and brochures available under the Our Products section of the website or call 724-338-4100.
Healthcare Business Strategy is a FREE monthly brief that presents analysis of important issues and developments affecting healthcare business today. If you would like to be added to our email distribution list, please submit your email address to the "Subscribe to MFA Briefs" section at the bottom of this page.