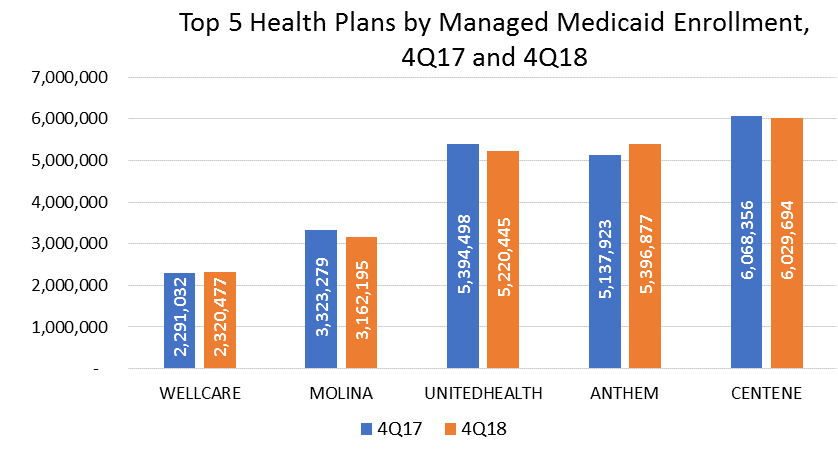
Key Provider Centene Continued as the Medicaid Segment Leader by Membership for 2018
April 22, 2019
Source: Health Coverage Portal TM, Mark Farrah Associates, presenting data from the National Association of Insurance Commissioners (NAIC) and the California Department of Managed Health Care (CA DMHC).
- Centene lead the managed Medicaid market with over 6.0 million members in 4Q17 and 4Q18. In March 2019, Centene announced a proposal to acquire WellCare for over $15 billion. If approved, it would create a leading health care giant specializing in government-sponsored programs and ACA state insurance marketplaces. The acquisition is expected to close in June of 2020.
- Anthem was one of only two plans in the top five to experience growth by nearly 259,000 members from approximately 5.1 million members in 4Q17 to nearly 5.4 million enrolled in 4Q18.
- UnitedHealth experienced the largest actual YOY loss in membership by 174,000 members, with 4Q18 enrollment figures at 5.2 million according to the NAIC.
- Molina’s 2018 year-end enrollment stood at 3.2 million, a decrease of 4.8% from 4Q17.
- WellCare, the only other health plan in the top 5 to experience growth, increased managed Medicaid by 1.3% to end 2018 with 2.3 million members.
Please note: There are reporting differences in Medicaid membership between the NAIC and SEC due to segment definitions, state laws and other causes. This analysis is focused on the managed Medicaid market as reported to the NAIC. SEC 10K Medicaid membership for Centene was 8.4 million, Anthem reported 6.7 million, UnitedHealth reported approximately 6.5 million, Molina was nearly 3.4 million, and WellCare stood at 3.9 million.
About Mark Farrah Associates (MFA)
Mark Farrah Associates (MFA) is a leading data aggregator and publisher providing health plan market data and analysis tools for the healthcare industry. Our product portfolio includes Health Coverage Portal™, County Health Coverage™, Medicare Business Online™, Medicare Benefits Analyzer™, and Health Plans USA™. For more information about these products, refer to the informational videos and brochures available under the Our Products section of the website or call 724-338-4100.
Healthcare Business Strategy is a FREE monthly brief that presents analysis of important issues and developments affecting healthcare business today. If you would like to be added to our email distribution list, please submit your email to the "Subscribe to MFA Briefs" section at the bottom of this page.