An Analysis of Profitability for the Individual and Small Group Health Insurance Markets in 2021
July 12, 2022
Health plans across the country submitted their Supplemental Health Care Exhibits (SHCE) on April 1, 2022, as part of the 2021 National Association of Insurance Commissioners’ (NAIC) annual financial statements. The SHCE contains financial performance metrics, membership, and preliminary MLRs (Affordable Care Act’s (ACA’s) Medical Loss Ratios) at the state level. Subscribers to Mark Farrah Associates’ (MFAs) Health Coverage PortalTM or the SHCE & MLR Data have access to this important information. MFA examined some key findings from its latest analysis of the SHCE, including a focus on performance within Individual and Small Group comprehensive insurance segments. Plans in these two segments face the added constraint of a standard (minimum) MLR.
Segment Profitability Overview
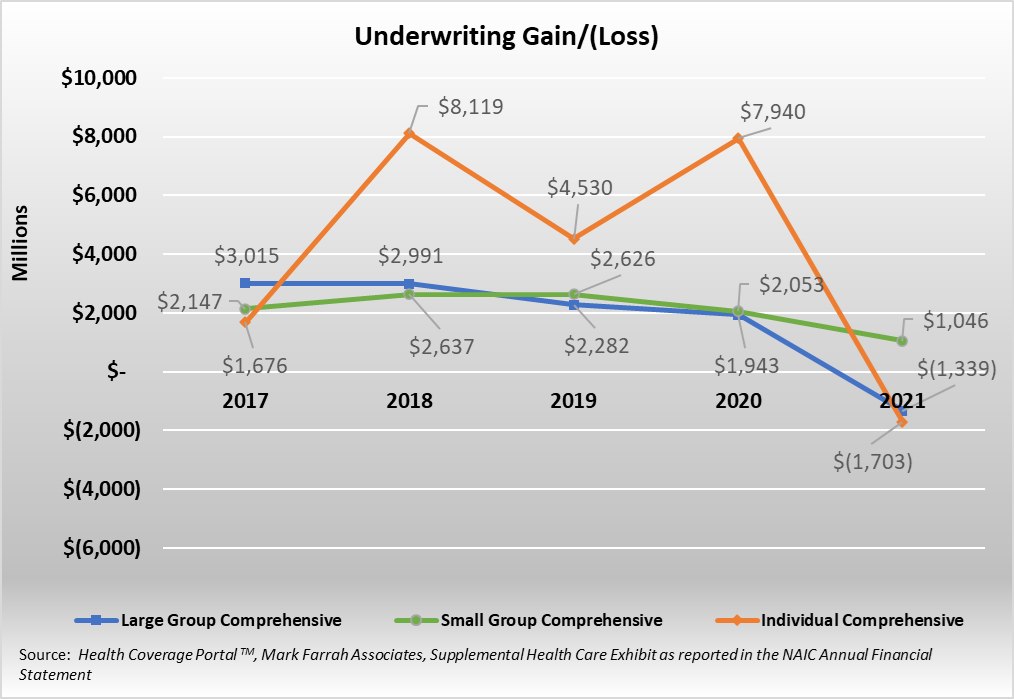
Beginning with the individual segment, year-end 2021 membership was almost 13.2 million members, up from 11.3 million members in 2020. This is its highest point since 2016. While segment membership is trending up, segment profitability for health insurance companies reached its lowest point since 2017, with a $1.7 billion underwriting loss.
While the declines in small group segment membership continued in 2021, down year-over-year by 5%, to 9.6 million, the segment remains more profitable per member than the large group segment. The segment has reported over $10 billion in cumulative underwriting gains since 2017. While the underwriting gain of over $1 billion was down by 49% from 2020, the segment remained profitable, while both the individual and large group segments reported losses.
Individual Comprehensive Segment
After four years of profitability, the Individual segment reported a loss of $1.7 billion in 2021 as members caught up on covid-related delays in health care. While profits were down, the segment experienced enrollment growth of 16%, to 13.2 million members for 2021. Premiums increased 1.6%, to a segment average of $526.8 premiums PMPM (per member per month**). However, medical claims jumped 19.5% on a PMPM basis for 2021 after dropping 8.6% during 2020. The average medical claims PMPM was $482 for 2021.
Focusing on the segment leaders for this analysis, we will look at four-year trends in membership, medical claims incurred PMPM, adjusted premium PMPM, and their SHCE-reported MLR**.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit as reported in the NAIC Annual Financial Statement
Segment leadership is based on 2021 SHCE-reported membership by company. Centene continued its growth within the segment, reporting a 7.4% increase in individual enrollment. Molina jumped into the top 5 for 2021 with a 143% increase in membership with strong growth in all their markets, with Texas leading the way with almost 250K new members. From 2020 to 2021, the entire Individual segment grew by 1.8 million members.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit and the Statement of Revenue and Expenses as reported in the NAIC Annual Financial Statement
Health insurers reported a large increase in spending on medical costs for the 2021 Individual segment. Average incurred claims PMPM increased from $404 in 2020 to $482 in 2021, a 19.5% increase. HCSC (Health Care Service Corporation) experienced the largest increase, rising 67% to $572 PMPM in 2021 from $343 PMPM in 2020. Molina reported the lowest growth in incurred claims of the leaders, increasing only 6% to $296 PMPM.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit and the Statement of Revenue and Expenses as reported in the NAIC Annual Financial Statement
Premiums PMPM grew between 2020 and 2021 by 1.6% but are still below the 2019 peak of $530 PMPM. Nevertheless, 2021’s premiums PMPM of $527 PMPM are 128% greater than before the impact of the ACA. For 2021, Centene reported a 12.6% increase in premium PMPM, the largest among the top 5 plans. Molina’s premium PMPM dropped by almost 10%, impacted significantly by $736 million in accrued risk adjustment payments due.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit as reported in the NAIC Annual Financial Statement
The Medical Loss Ratio (MLR) illustrates the relationship between premiums and medical costs. While premiums only grew slightly in 2021, medical expenses increased significantly leading to approximately 77% of plans reporting increases in their MLRs for 2021. For the segment leaders, HCSC experienced a large increase in their average MLR due in part to significant risk corridor revenue (from previous years) that was recognized in 2020, leading to an abnormally low MLR.
It is important to note that Mark Farrah Associates is reporting all data as filed with the NAIC (National Association of Insurance Commissioners) in the annual SHCE. We are not adjusting the data to account for differences in the number of reporting plans between 2017 and 2021. We did adjust our data to account for one significant late filing 2021 plan. For purposes of this analysis, MFA has calculated a weighted average MLR** based upon adjusted premiums.
Small Group Comprehensive Segment
While the Small Group segment continues to lose membership, down another 5.1% for 2021 with small businesses opting to either self-insure or drop health insurance coverage for their employees, overall segment profitability remains strong. Focusing on the segment leaders for this analysis, we will look at four-year trends in membership, claims incurred PMPM, adjusted premium PMPM and segment leaders’ SHCE-reported MLR.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit as reported in the NAIC Annual Financial Statement
The five segment leaders, based on membership, include UnitedHealth, HCSC, Anthem, CareFirst and Blue Cross Blue Shield Michigan (BCBS MI). UnitedHealth experienced the largest decrease in membership of the top plans, reporting a 5.9% drop in enrollment. HCSC, CareFirst and BCBS MI all stood out from the segment, as a whole, by posting gains in membership. Overall, the segment membership was down 517K members for 2021.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit as reported in the NAIC Annual Financial Statement
Average incurred claims PMPM increased from $392 in 2020 to $448 in 2021, a 14% increase. CareFirst reported the largest increase in incurred claims PMPM among the segment leaders with a 11.3% year-over-year change.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit as reported in the NAIC Annual Financial Statement
Average adjusted premium PMPM for the segment rose from $472 in 2020 to $521 in 2021, a 10.4% increase. This represents the largest year-over-year increase since the onset of the ACA. All five segment leaders reported increases in premiums PMPM for 2021. UnitedHealth’s premium PMPM increased 13.4% over 2020, the only plan in the top 5 that outpaced the average segment increase.
Source: Health Coverage Portal TM, Mark Farrah Associates, Supplemental Health Care Exhibit as reported in the NAIC Annual Financial Statement
Overall, the leading plans have been able to better manage MLRs within the Small Group segment as compared to larger challenges in the Individual segment. For 2021, most notable among the segment leaders was UnitedHealth’s 82.7% average MLR, a notable decrease from 2020 due to premium increases.
Conclusion
For both the Small Group and Individual segments, underwriting gains made during the height of the pandemic were at least in part lost during 2021, as members caught up on delayed health care. Premium growth, for the Individual segment has stabilized with minimal change since 2019, which is good news for consumers. While both segments have been impacted by the pandemic-influenced seesawing of medical spending between 2020 and 2021, both segments were profitable for insures over the two-year combined period. The growth of enrollment in the Individual segment in 2020 continued into 2021 and is a notable development, most likely caused by the economic/employment changes brought on by COVID-19. This growth has continued through the first quarter of 2022. Mark Farrah Associates will have more to report on 2022 enrollment and profitability trends in the coming months.
* PMPM – Per Member Per Month is an amount divided by member months; one member enrolled for 12 months equals 12 member months.
** Weighted Average MLR – For analysis purposes, Mark Farrah Associates calculated average preliminary MLRs weighted on the adjusted premiums for each company by segment. The MLRs used in the calculation are average ratios based upon 2018– 2021 as reported in the NAIC’s Supplemental Health Care Exhibit.
SCHE Data
The data used in this analysis brief was obtained from Mark Farrah Associates' Health Coverage Portal TM using Supplemental Health Care Exhibit (SHCE) data as reported in the NAIC Annual Financial Statement. Each year, MFA updates its products with the latest SHCE data. Additionally, MFA maintains financial data as well as enrollment and market share for the health insurance industry in the subscription-based Health Coverage Portal TM.
For more information about our products, refer to the product videos and brochures available on Mark Farrah Associate’s website or call 724-338-4100.
About Mark Farrah Associates (MFA)
Mark Farrah Associates (MFA) is a leading data aggregator and publisher providing health plan market data and analysis tools for the healthcare industry. Our product portfolio includes Health Coverage Portal™, County Health Coverage™, Medicare Business Online™, Medicare Benefits Analyzer™, 5500 Employer Health PLUS, and Health Plans USA™. For more information about these products, refer to the informational videos and brochures available under the Our Products section of the website or call 724-338-4100.
Healthcare Business Strategy is a FREE monthly brief that presents analysis of important issues and developments affecting healthcare business today. If you would like to be added to our email distribution list, please submit your email address to the "Subscribe to MFA Briefs" section at the bottom of this page.